What did your survey tell us about migraine and fibromyalgia?
At the beginning of this year, we asked you to help tell us more about the many ways migraine impacts your life. Among the many questions we asked, there were questions about other types of pain you might also have. Fibromyalgia is a chronic pain condition experienced as widespread body pain, with sleep problems, fatigue, depression, and digestive problems. We know people with migraine often have other pain conditions, like fibromyalgia. If you have fibromyalgia, it's important to recognize it so you can get it treated.
Fibromyalgia is a challenging pain problem. Many doctors never learned about fibromyalgia during training and there are a lot of misconceptions about this diagnosis. It usually takes several years of symptoms and seeing many doctors before people finally learn they have fibromyalgia. In an effort to help make the diagnosis easier, the American College of Rheumatology put together new criteria to help doctors recognize this condition. In the survey, we asked you to complete questions so we could determine how many of you with migraines might also have fibromyalgia.
What did we learn from the survey?
In January and February, 1446 adults with migraine took our online survey. Among those, 24 percent -- nearly one in four migraineurs -- met criteria for having fibromyalgia. We decided to investigate the differences between migraine sufferers with and without fibromyalgia. Here's what we found:
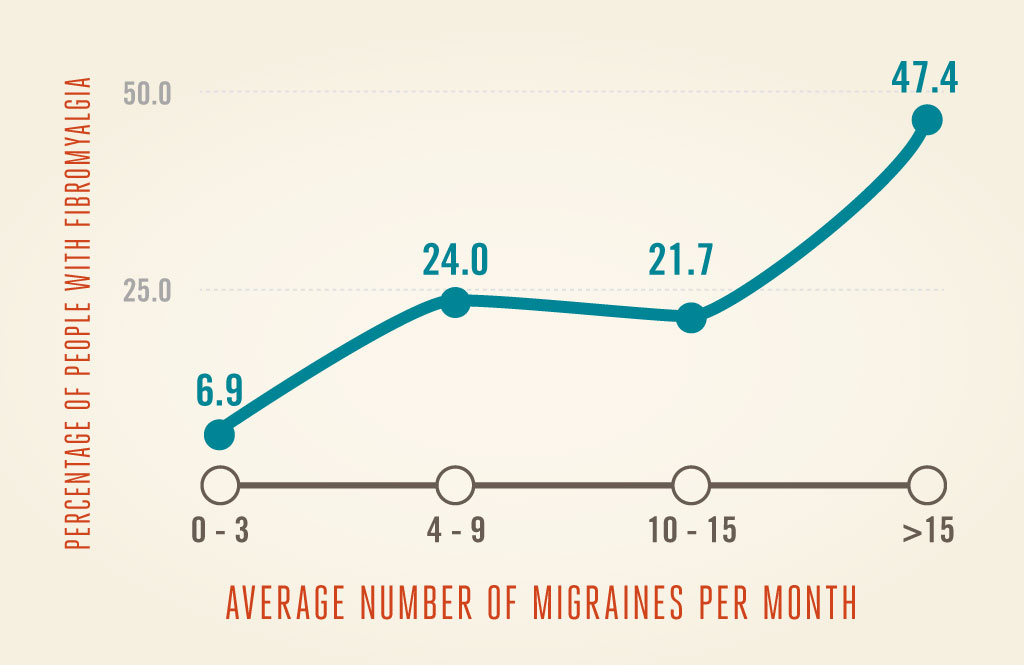
- Migraine frequency was higher among migraineurs who also had fibromyalgia.
- Most migraineurs without fibromyalgia had 2 or fewer migraines per week.
- Most migraineurs with fibromyalgia had chronic migraine, having 15 or more migraines per month.
- Fibromyalgia symptom severity also increased as the number migraine attacks per month increased.
- People with both migraine and fibromyalgia were more likely to have mood problems.
- One in three migraine sufferers without fibromyalgia had depression.
- One in three migraineurs without fibromyalgia had anxiety.
- Two in three migraineurs with fibromyalgia were depressed.
- Two in three migraineurs with fibromyalgia had anxiety problems.
- As fibromyalgia severity increased, mood correspondingly worsened.
What does this teach you about migraine and fibromyalgia?
This study shows that migraine and fibromyalgia often go hand-in-hand. If you typically have migraines more than twice a week, you might want to see if you may also have fibromyalgia. If you have widespread aches and pain, mood problems, fatigue, or trouble sleeping, you may have fibromyalgia. You can complete the fibromyalgia screening questionnaire by clicking here. If you think you have fibromyalgia, be sure to talk to your doctor about how fibromyalgia is treated.
Community Poll
Do you feel comfortable advocating for yourself to your healthcare provider?
Join the conversation